In a major stride towards enhancing global epidemic preparedness, Drs. Victoria May Mendoza and Renier Mendoza of the UP-Diliman College of Science Institute of Mathematics (UPD-CS IM) have provided key findings on the dynamics of the Mpox (monkeypox) spread. In collaboration with South Korean researchers, the team developed an innovative algorithm to investigate the pivotal role of self-reporting and contact tracing in the early stages of Mpox transmission via simulations.
Their findings, published in the Journal of Medical Virology, showed that the most crucial element affecting the size of an outbreak and its potential duration is the behavior of the primary case—that is, the infected person carrying the disease into a community, and whether or not they report their status for medical attention.
The study followed as a result of a sudden Mpox outbreak in non-endemic countries in May 2022. Although the majority of the infected had had no history of travelling to the endemic areas of central and western Africa, the disease continued to spread, and more and more cases were still being reported worldwide.
In South Korea, however, the first case of an individual diagnosed with Mpox had immediately self-reported in June 2022. After travelling to Europe and returning in the same month, the primary case informed the Korea Disease Control and Prevention Agency (KDCA) of his symptoms and contact history. Subsequently, there were no other recorded secondary infections of Mpox within the country.
Based on stochastic chemical kinetics
To study this scenario and the other factors affecting the potential outbreak of Mpox in a non-endemic country, the team used a mathematical model based on Gillespie’s stochastic chemical kinetics.
Stochastic models are quantitative techniques that take into account random variables when predicting possible outcomes. While these have commonly been used to analyze the effects of other infectious diseases, this marked the first time that a stochastic model was used to simulate the spread of Mpox in a non-endemic country.
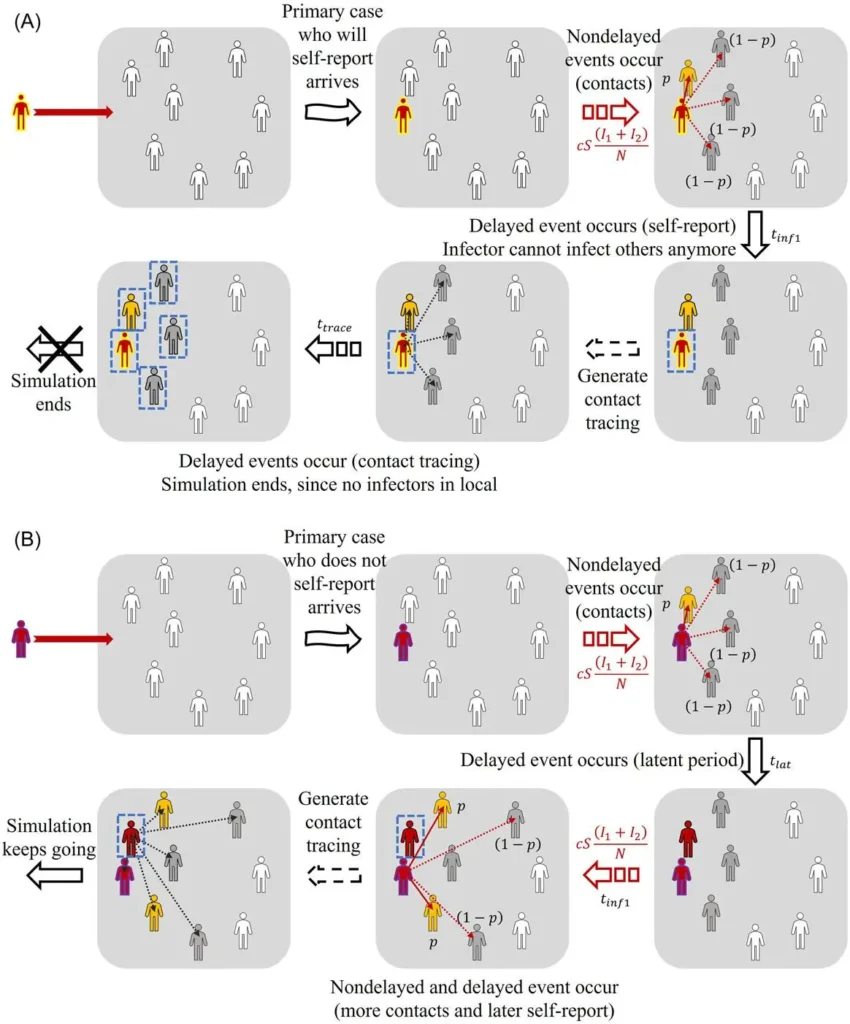
In this manner, their algorithm considered random fluctuations in human behavior and subsequent delayed contact tracing. They then set up 8 scenarios for their study, running 100,000 simulations in each to better understand the significance and impact of the primary case’s self-reporting or lack thereof.
Through these simulated outbreaks, they projected the average numbers of infected individuals depending on whether the primary case self-reported or not. In the scenario wherein the primary case self-reported, the number of infected individuals only increased by 11%. But in the scenario wherein the primary case did not self-report, thereby further delaying contact tracing, the number of infected individuals increased by up to 40%.
The large difference in results served as both clear evidence and cautionary tales of the dangers of unreported cases. By understanding the impact of the primary case’s and infectees’ behavior, the study provides a more intuitive analysis that healthcare authorities may use as guiding information in the management and detection of possible Mpox outbreaks in the future.
However, the researchers believed that one of the many factors dissuading people from seeking medical help—therefore greatly affecting attempts to mitigate disease—was stigma.
“The social media coverage about Mpox spread directly or indirectly generates racist and homophobic stereotypes that worsen stigma,” they explained in their paper. They emphasized that approaches to encouraging self-reporting should be based on rights and evidence to avoid situations of hidden infected cases.
“Healthcare authorities must ensure confidentiality of confirmed cases and individuals under investigation, and access to health services. Moreover, prompt case finding and information campaigns must be conducted,” they urged.
The World Health Organization (WHO) now uses the term Mpox due to the racist and stigmatizing language surrounding the disease online following the 2022 outbreak. The virus itself is transmittable either through animal-to-human or human-to-human contact with bodily fluids or any contaminated material. For the 2022 outbreak, the symptoms were largely flu-like, with rashes that started around the genital area—but unlike the rashes typical to Mpox, they appeared more similar to measles or other noninfectious conditions. (Story by Maria Alexandra Marmol, UPD-CS Science Communications; image courtesy of UPD-CS Science Communications)